Diagnosis of Disease
Diagnosis of parasitic disease through DNA probe
Probes used for diagnosis of pathogens contain the most specific DNA sequences of genetic material of parasite. The specificity lies in such a way that the other related species or strain do not contain those sequences. These unrelated unspecific sequences of parasite are first recognized by using DNA hybridization technique. Then a DNA sequence, not present in any species, is identified, cleaved by using restriction enzymes, and inserted into a cloning vector (plasmid). The bacterial cells are transformed by the recombinant vector. The tranformants are multiplied. Finally, the foreign DNA fragments are retrieved from the host cells. The DNA sequences of the parasite, thus obtained, are labeled with radioisotope and used as a probe. The probe can also be chemically synthesized. Following are the steps for diagnosis of a particular disease :
- Isolate the parasite from the infected tissue of the patient. Extract the DNA from parasite and purify it
- Break the DNA by using restriction enzymes to get the DNA fragments of varying size
- Electrophorise the DNA solution of different length by using agarose gel just to get a smear of DNA
- Attach the DNA smear to more firmer support by Southern blotting techniques. Thus the filter paper carries the exact replica of the DNA adhered to it
- Hybridize the immobilized DNA on filter paper by incubating it with radiolabeled probe. Probe DNA complementary to certain DNA sequences of parasite DNA sticks to it and forms the hybrid
- Wash the filter paper to remove unhybridized probe. Keep the filter in contact of x-ray film. Dark bands appear where DNA probe had hybridized the specific target sequence. Thus, a parasitic disease is diagnosed positive. If dark bands on x-ray film do not appear, the absence of parasite is noted.
Monoclonal antibodies Antibodies are proteins synthesized in blood against specific antigens just to combat and give immunity in blood. They can be collected from the blood serum of an animal. Such antibodies are heterogeneous and contain a mixture of antibodies (i.e.polyclonal antibodies). Therefore, they do not have characteristics of sepcificity. If a specific lymphocyte, after isolation and culture in vitro, becomes capable of producing a single type of antibody which bears sepcificity against specific antigen, it is known as ‘monoclonal antibody’. Due to the presence of desired immunity, monoclonal antibodies are used in the diagnosis of diseases.
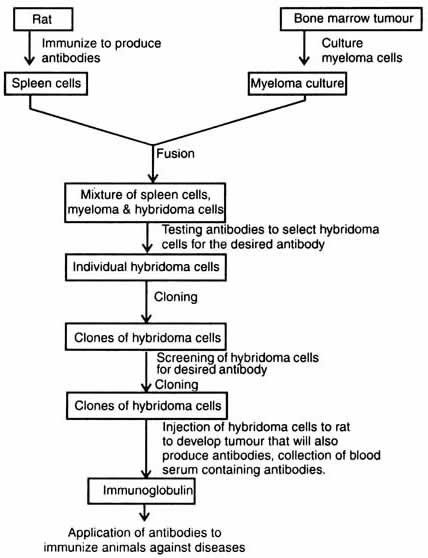
Hybridoma. Cesal Milstein of Argentina tried to culture myeloma cells. In 1973, in collaboration with Cotton, he succeeded to fuse rat and mouse myeloma cells with the result of production of hybrid cells. The hybrid cells secreted the immunoglobulins which consisted of several types of polypeptides. In 1974, George Kohler and Milstein successfully isolated clones of cells from the fusion of two parental cell lines i.e. between lymphocyte from spleen of mice immunized with red blood cells from sheep and myeloma cells. These cells were maintained in vitro and produced antibodies. The antibodies for specific antigens immunized the myeloma cells (Kohler and Milstein, 1975). Moreover, the hybrid cells maintained the character of lymphocyte to secrete antibodies, and of myeloma cells to multiply in culture. These hybrid cell lines (cell clones) are known as hybridomas which are capable of producing unlimited supply of antibodies. For the discovery of production of monoclonal antibodies Kohler and Milstein along with Neils Jerne were awarded Nobel Prize in 1984, in physiology and medicine. Now, techniques are developed to obtain antibodies from hybridoma culture (Fig. 5.7).
Monoclonal antibodies are produced against a variety of proteins, glycoproteins, glycolipids, nucleic acids and chemically defined groups linked to protein carriers. Possibility of success is related to the number of antibody forming cells in spleen at the time of fusion.
This, in turn, depends on immunogenicity of the antigen used. For example, a mouse spleen contains about 108 nucleated cells. Sheep red blood cells (SRBC) act as immunogens and stimulate the replication and differentiation of antibody forming cells. At the time of secondary response each spleen may contain 106 cells producing antibody against SRBC. Among 2 x 105 spleen cells only one hybrid cell is generated.
About 500 hybrid cells per spleen can be obtained where five of these produce specific antibody (Kwan et al, 1980). The cells growing on culture and producing sufficient amount of monoclonal antibodies can be frozen. The cells are collected through centrifugation and resuspended at a density of 107 cells per ml freezing medium in cold at 0J°C. Samples (0.7-1.0 ml) poured in sterile glass vials are sealed and stored at 80°C (Kwan et al, 1980).
In India, a hybridoma laboratory has been set up with indigenous material at the Cancer Research Institute (CRI), Bombay. The first experiment conducted at C.R.I, was an attempt to develop leukemia cell reactive monoclonal antibody.
- In diagnosis of ABO blood groups, cancer, pregnancy, allergies, viral diseases and certain, hormones;
- Immunopurification of interferon from a mixture of substances;
- Treatment of disease, for example, tumour;
- Organ transplantation.
- When the other methods and surgery get failed to diagnose cancer at very important places, use of monoclonal antibodies is suggested. Monoclonal antibodies are labeled with radioactive chemical such as I125 and cancer patients are injected with these. After some times gamma scan is done. Dark spots appear where nodules of tumour have been formed. Now, use of drugs, radiation or surgery is suggested to patients.
- One of the successfully used methods is the coupling of monoclonal antibodies with toxins such as ricin. This is called as magic bullet treatment or targeted drug delivery (see gene therapy). It is found very successful in cleaning the bone-marrow of leukemic cells.
There are as many as 2,500 genetic defects known to occur in human beings. Some of them (e.g. phenylketonuria and haemophilia) have been cured but most of them are not understood. If a pregnant woman bears a child with a genetic defect, often she is advised to abort it but not to give birth to genetically defected child. Thus, the technique of diagnosis and thereby suggestion for abortion of a genetically defected child is known as antenatal diagnosis. The genetically determined defects of function or synthesis of human haemoglobin is known as haemoglobinopathies
The inherited haemoglobinopathies are : (i) the structural variants where till now 300 amino acid variants are identified, and (ii) the thalassaemias, a condition characterized by reduced or absent synthesis of a or b- globin chain, a and b-thalassaemia respectively.
The foetus fluid also contains foetally derived fibroblasts which serve, with or without additional culture, as a source of tissue for preparation of foetal DNA. Structural analysis of DNA is done by (a) isolation of all the globin genes as recombinant DNA molecules, and cloning in bacteria, or (b) without cloning the recombinant DNA in -bacteria directly by "Southern Blotting Technique" (Southern, 1975), and (c) linked polymorphism. A detailed account of DNA analysis of structural genes is given by Little (1981). There are about 35 diseases which have been identified by antenatal diagnosis. This method helps in suggesting the abortion of defected baby, and if possible, to cure . It can be recommended for gene therapy as well. Thus, the antenatal diagnosis is applied for both genetic counseling and gene therapy.