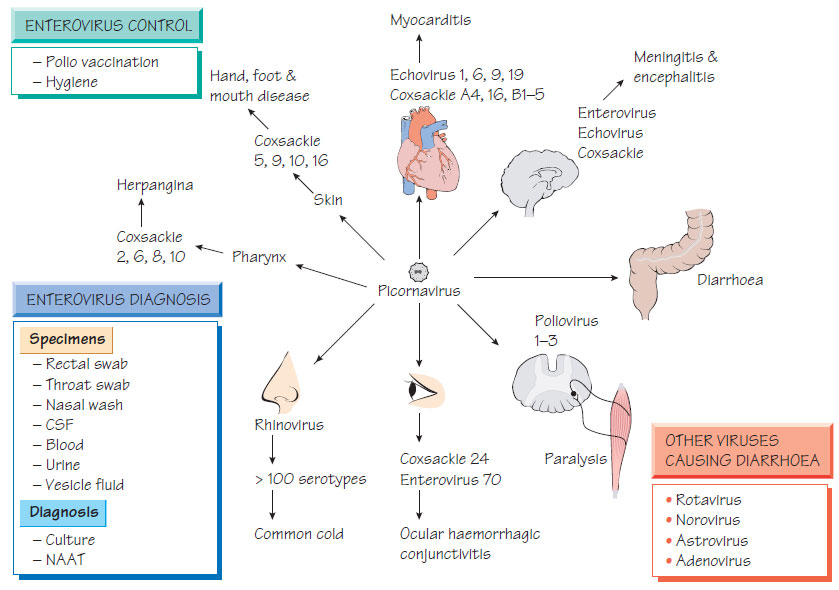
Enterovirus and viruses that infect the gastrointestinal tract
EnterovirusEnteroviruses are picornaviridae with three serotypic groups: poliovirus, coxsackievirus and enteric cytopathic human orphan (ECHO) virus (echovirus). Later isolates have been designated with a number (e.g. enterovirus 68-72). Enteroviruses are unenveloped, icosahedral, positive-sense RNA viruses that encode for four proteins.
Pathogenesis
- The virus enters cells by a specific receptor that differs for different virus types, therefore defining tissue tropism.
- The virus is usually acquired via the intestinal tract, causing subsequent viraemia and invasion of reticuloendothelial cells.
- Secondary viraemia leads to invasion of target organs (e.g. meninges, spinal cord, brain or myocardium).
- Poliovirus appears to spread along nerve fibres; if significant multiplication occurs within the dorsal root ganglia, the nerve fibre may die, with resultant motor paralysis.
Epidemiology
- Enteroviruses are spread by the faecal-oral route.
- In developing countries infection occurs early in life; it occurs later in industrialized countries.
- Infection can occur in parents and carers of infants who have received the live vaccine.
Polio may present as a minor illness (abortive polio), as aseptic meningitis (non-paralytic polio), with lower motor neurone damage and paralysis (paralytic polio), or as a late recrudescence of muscle wasting that occurs sometimes decades after the initial paralytic polio (progressive postpoliomyelitis muscle atrophy). In paralytic polio, muscle involvement is maximal within a few days after commencement of the paralysis; recovery may occur within 6 months.
- Aseptic meningitis (see Infections of the central nervous system) and, rarely, severe focal encephalitis or general infection may present in neonates.
- Herpangina, a self-limiting, painful, vesicular pharyngeal infection, is caused by some types of coxsackievirus.
- Coxsackie B causes acute myocarditis (see Endocarditis, myocarditis and pericarditis).
- Hand, foot and mouth disease is characterized by a vesicular rash of the palms, mouth and soles that heals without crusting.
- Diagnosis is usually by nucleic acid amplification test (NAAT) of CSF, throat swab and faecal specimen.
- Culture is available.
- The multiplicity of serotypes makes serological Diagnosis impractical.
- Treatment is supportive care but pleconaril shows benefit in the treatment of enteroviral meningitis. Artificial ventilation may be required in the case of polio.
Prevention
Two vaccines are available: the oral live attenuated Sabin and the killed parenteral Salk vaccine. Now that polio is limited to a few countries, the inactivated poliovirus vaccine (IPV) is used.
Rhinovirus
- Rhinovirus is responsible for the common cold.
- More than 100 serological types exist.
- It has a short incubation period (2-4 days).
- The virus is excreted whilst symptoms are present.
- Transmission is by contact.
The virus infects the upper respiratory tract, invading only the mucosa and submucosa. The primary symptoms of headache, nasal discharge, upper respiratory tract inflammation and fever may be followed by secondary bacterial infections such as otitis media and sinusitis. Infection occurs worldwide with a peak incidence occurring in the autumn and winter. Immunity after infection is poor because of the multiplicity of serotypes. Ruprintrivir given by nasal spray has been shown to shorten symptoms in clinical trials. A vaccine is impractical.
Rotaviruses are unenveloped viruses that contain 11 doublestranded RNA segments coding for nine structural proteins and several core proteins.
Pathogenesis
Rotaviruses infect small-intestinal enterocytes; damaged cells are sloughed into the lumen, releasing viruses. Diarrhoea is caused by poor sodium and glucose absorption by the immature cells that replace the damaged enterocytes.
Epidemiology
Rotaviruses are the main cause of viral diarrhoea, occurring usually in children between 6 months and 2 years of age. Morbidity is highest in the young in developing countries. There are seasonal peaks in the winter in temperate countries. Antibody to the virus does not confer immunity to further infection.
- Diagnosis by reverse transcriptase NAAT is most sensitive.
- Antigen can be detected by enzyme immunoassay (EIA).
- The virus can be visualized by electron microscopy (EM).
Treatment and Prevention
Treatment is symptomatic and supportive. The risk of infection can be reduced by provision of adequate sanitation. Vaccines have been introduced into countries where rotavirus morbidity and mortality are high.
Noroviruses are caliciviruses that cause outbreaks of acute diarrhoea and vomiting in hospitals and care homes, on cruise liners and in other confined communities. Infection is transmitted by the faecal-oral and aerosol routes with symptoms developing after a short incubation period (24-48 h). The viruses can be divided into five genogroups. Astroviruses are small spherical particles; more than five serotypes have been recognized. Virus replication occurs in the mucosal epithelium of the small intestine, which results in broadening and flattening of the villi and hyperplasia of crypt cells.
- Infection usually causes a self-limiting, acute diarrhoeal illness.
- It can present with sudden-onset, projectile vomiting and explosive diarrhoea.
- Sudden outbreaks of norovirus infection may occur in institutions, requiring the units to close to new admissions.
- Diagnosis is made by NAAT.
- Sequencing is required for epidemiological purposes and to monitor the design of future NAAT detection assays.
- Prevention is by isolation, ward closure and good hand-washing technique.