Vertebrate Kidney Function
Vertebrate Kidney
Function
The vertebrate kidney is part of many interlocking mechanisms that maintain homeostasis. The kidney plays a prominent role in this regulatory council because it is the principal organ that regulates the volume and composition of the internal fluid environment. While we commonly describe the vertebrate kidney as an organ of excretion, the removal of metabolic wastes is incidental to its regulatory function. The organization of kidneys differs somewhat in different groups of vertebrates, but in all the basic functional unit is the nephron, and urine is formed by three well-defined physiological processes: filtration, reabsorption, and secretion. The following discussion focuses mainly on the mammalian kidney, which is the most completely understood regulatory organ.
The two human kidneys are small organs comprising less than 1% of the body weight. Yet they receive a remarkable 20% to 25% of the total cardiac output, some 2000 liters of blood each day. This vast blood flow is channeled to approximately 2 million nephrons, which make up the bulk of the two kidneys. Each nephron begins with an expanded chamber, the renal corpuscle, containing a tuft of capillaries called the glomerulus (glomer 'yoo-lus). Blood pressure in the capillaries forces a protein-free filtrate into a renal tubule, consisting of several segments that perform different functions in the process of urine formation. The filtrate passes first into a proximal convoluted tubule, then into a long, thin-walled loop of Henle, which drops deep into the inner portion of the kidney (the medulla) before returning to the outer portion (the cortex) where it joins a distal convoluted tubule. From the distal tubule the fluid empties into a collecting duct which drains into the renal pelvis. Here the urine is collected before being carried by the ureter to the urinary bladder. These anatomical relationships are shown in Figure 32-10.
The urine that leaves the collecting duct is very different from the filtrate produced in the renal corpuscle. During its travels through the renal tubule and collecting duct, both the composition and concentration of the original filtrate change. Some solutes such as glucose and sodium have been reabsorbed while other materials, such as hydrogen ions and urea, have been concentrated in the urine.
The nephron, with its pressure filter and tubule, is intimately associated with blood circulation (Figure 32-11). Blood from the aorta enters each kidney through a large renal artery, which divides into a branching system of smaller arteries. The arterial blood reaches the renal corpuscle through an afferent arteriole and leaves by way of an efferent arteriole. From the efferent arteriole the blood travels to an extensive capillary network that surrounds and supplies the proximal and distal convoluted tubules and the loop of Henle (Figure 32-10). This capillary network provides a means for the pickup and delivery of materials that are reabsorbed or secreted by the kidney tubules. From these capillaries blood is collected by veins that unite to form the renal vein. This vein returns the blood to the vena cava.
Glomerular Filtration
Let us now return to the glomerulus, where the process of urine formation begins. The glomerulus acts as a specialized mechanical filter in which a protein-free filtrate of the plasma is driven by the blood pressure across the capillary walls and into the fluidfilled space of the renal corpuscle. Solute molecules small enough to pass through the slit pores of the capillary wall are carried through with the water in which they are dissolved. Red blood cells and plasma proteins, however, are withheld because they are too large to pass through these pores (Figure 32-12).
The filtrate continues through the renal tubular system where it will undergo extensive modification before becoming urine. Human kidneys form approximately 180 liters (nearly 50 gallons) of filtrate each day, a volume many times exceeding the total blood volume. If this volume of water and the valuable nutrients and salts it contains were lost, the body would soon be depleted of these compounds. Depletion does not happen because nearly all of the filtrate is reabsorbed. The final urine volume in humans averages 1.2 liters per day.
Conversion of filtrate into urine involves two processes: (1) modification of the composition of the filtrate through tubular reabsorption and secretion, and (2) changes in the total osmotic concentration of the urine through the regulation of water excretion.
The vertebrate kidney is part of many interlocking mechanisms that maintain homeostasis. The kidney plays a prominent role in this regulatory council because it is the principal organ that regulates the volume and composition of the internal fluid environment. While we commonly describe the vertebrate kidney as an organ of excretion, the removal of metabolic wastes is incidental to its regulatory function. The organization of kidneys differs somewhat in different groups of vertebrates, but in all the basic functional unit is the nephron, and urine is formed by three well-defined physiological processes: filtration, reabsorption, and secretion. The following discussion focuses mainly on the mammalian kidney, which is the most completely understood regulatory organ.
The two human kidneys are small organs comprising less than 1% of the body weight. Yet they receive a remarkable 20% to 25% of the total cardiac output, some 2000 liters of blood each day. This vast blood flow is channeled to approximately 2 million nephrons, which make up the bulk of the two kidneys. Each nephron begins with an expanded chamber, the renal corpuscle, containing a tuft of capillaries called the glomerulus (glomer 'yoo-lus). Blood pressure in the capillaries forces a protein-free filtrate into a renal tubule, consisting of several segments that perform different functions in the process of urine formation. The filtrate passes first into a proximal convoluted tubule, then into a long, thin-walled loop of Henle, which drops deep into the inner portion of the kidney (the medulla) before returning to the outer portion (the cortex) where it joins a distal convoluted tubule. From the distal tubule the fluid empties into a collecting duct which drains into the renal pelvis. Here the urine is collected before being carried by the ureter to the urinary bladder. These anatomical relationships are shown in Figure 32-10.
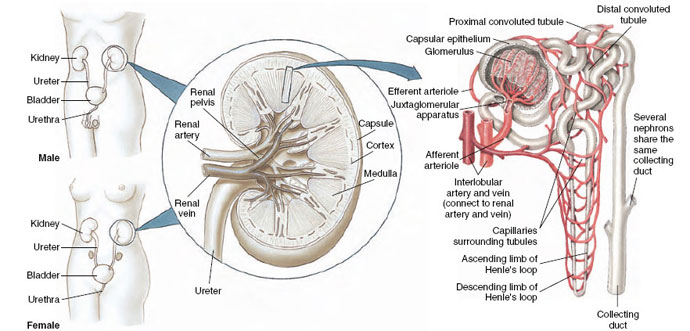 |
| Figure 32-10 Urinary system of humans, with enlargements showing detail of the kidney and a single nephron. |
The urine that leaves the collecting duct is very different from the filtrate produced in the renal corpuscle. During its travels through the renal tubule and collecting duct, both the composition and concentration of the original filtrate change. Some solutes such as glucose and sodium have been reabsorbed while other materials, such as hydrogen ions and urea, have been concentrated in the urine.
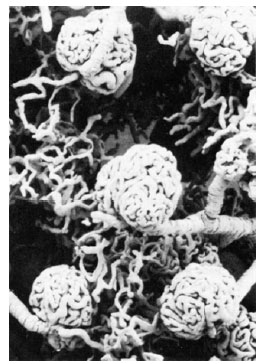 |
| Figure 32-11 Scanning electron micrograph of a cast of the microcirculation of the mammalian kidney, showing several glomeruli and associated blood vessels. The capsular epithelium, which normally surrounds each glomerulus, has been digested away in preparing the cast. |
The nephron, with its pressure filter and tubule, is intimately associated with blood circulation (Figure 32-11). Blood from the aorta enters each kidney through a large renal artery, which divides into a branching system of smaller arteries. The arterial blood reaches the renal corpuscle through an afferent arteriole and leaves by way of an efferent arteriole. From the efferent arteriole the blood travels to an extensive capillary network that surrounds and supplies the proximal and distal convoluted tubules and the loop of Henle (Figure 32-10). This capillary network provides a means for the pickup and delivery of materials that are reabsorbed or secreted by the kidney tubules. From these capillaries blood is collected by veins that unite to form the renal vein. This vein returns the blood to the vena cava.
Glomerular Filtration
Let us now return to the glomerulus, where the process of urine formation begins. The glomerulus acts as a specialized mechanical filter in which a protein-free filtrate of the plasma is driven by the blood pressure across the capillary walls and into the fluidfilled space of the renal corpuscle. Solute molecules small enough to pass through the slit pores of the capillary wall are carried through with the water in which they are dissolved. Red blood cells and plasma proteins, however, are withheld because they are too large to pass through these pores (Figure 32-12).
The filtrate continues through the renal tubular system where it will undergo extensive modification before becoming urine. Human kidneys form approximately 180 liters (nearly 50 gallons) of filtrate each day, a volume many times exceeding the total blood volume. If this volume of water and the valuable nutrients and salts it contains were lost, the body would soon be depleted of these compounds. Depletion does not happen because nearly all of the filtrate is reabsorbed. The final urine volume in humans averages 1.2 liters per day.
Conversion of filtrate into urine involves two processes: (1) modification of the composition of the filtrate through tubular reabsorption and secretion, and (2) changes in the total osmotic concentration of the urine through the regulation of water excretion.




